You are here
Radiotherapy Department
Head
Tomasz Rutkowski, PhD, MD
Registration phone: +48 32 278 80 45
CyberKnife - email: CyberKnife@io.gliwice.pl
Radiotherapy Department is
EUROPEAN REFERENCE CENTER FOR EDUCATION (RADIOTHERAPY)
(Varian Medical Systems International AG)
 The Radiotherapy Department is currently the largest and most modern institution of is kind in Poland and one of the largest in Europe. Most of the patients treated in our Department are irradiated using 3D conformal and dynamic techniques. All the linacs are equipped with image-guided radiation therapy systems to ensure high precision of the radiotherapy. Special respiratory gating systems have been implemented for radiotherapy of tumors with significant respiratory motion.
The Radiotherapy Department is currently the largest and most modern institution of is kind in Poland and one of the largest in Europe. Most of the patients treated in our Department are irradiated using 3D conformal and dynamic techniques. All the linacs are equipped with image-guided radiation therapy systems to ensure high precision of the radiotherapy. Special respiratory gating systems have been implemented for radiotherapy of tumors with significant respiratory motion.
Robotic microradiosurgery CyberKnife
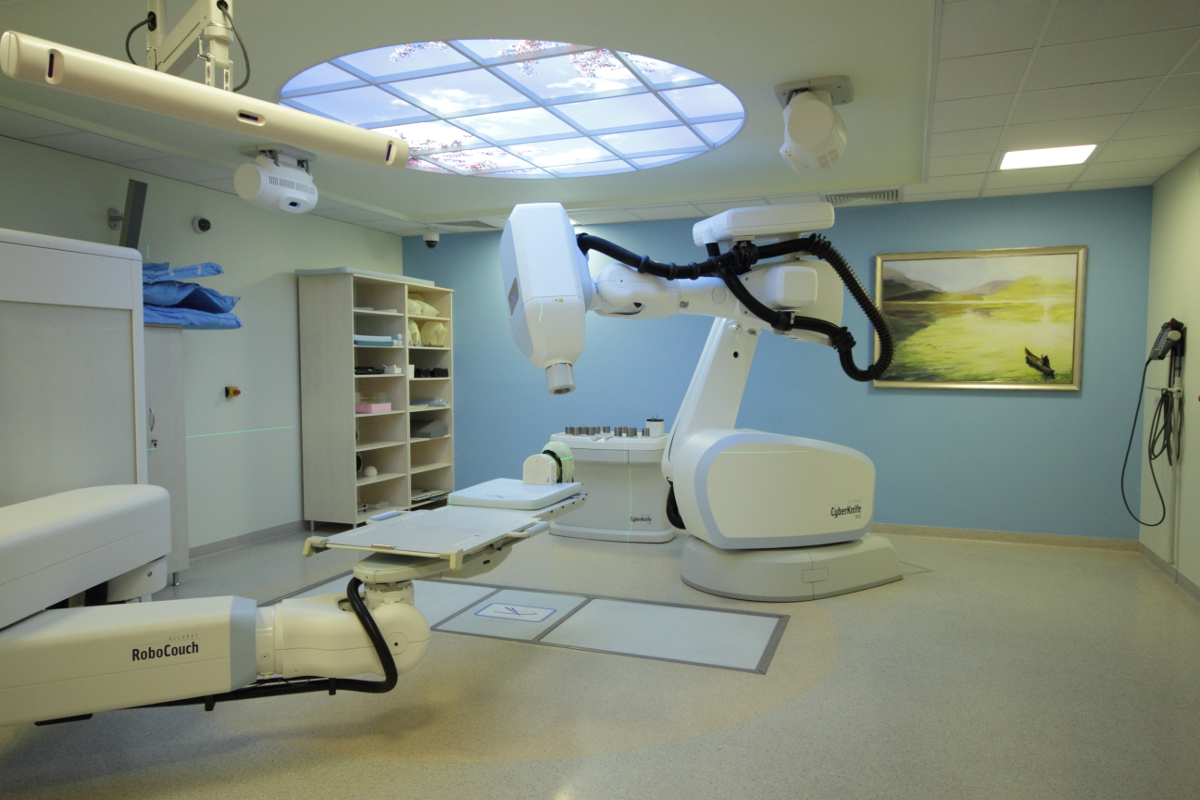
CyberKnife is a robot with incredible accuracy to 0.1 mm. The linac is mounted on an arm which can move in various directions since it rotates around several axes. Special collimators determine the size of the emitted beam allowing for irradiation of small tumors. Such a limited beam allows for high radiation doses for each application which otherwise – i.e. using standard linear accelerators - would not be safe for the patient. The method is called radiosurgery since it uses high doses of radiation; unlike surgery, however, it is noninvasive (does not cause destruction of tissue continuity), does not require anesthesia or rehabilitation, and the patient can continue his normal activity. Our Institute has pioneered this technology in Poland.
Treatment delivery
Depending on the case, one radiotherapy treatment takes between 45 minutes to two hours. During irradiation the patient is observed by medical personnel using five cameras and maintains voice contact through the intercom. The tumor site is monitored by the system continuously. When the patient moves, the system automatically adjusts the current position vs the patient reference position. The CyberKnife System ensures high precision treatment and prevents any error in the administration of the geometric beam. For locations with considerable respiratory mobility, the system keeps track of the patient's breathing and the moving tumor, closely following the lesion and avoiding irradiation of the surrounding healthy tissue. Once the therapy session is over, the patient can go home.
Typical indications:
- Brain tumors
- Liver and pancreatic tumors
- Lung tumors
- Early prostate cancers
- Tumors in locations characterized by high mobility of the tumor and the surrounding organs
- Spinal tumors
- Arteriovenous malformations of the brain
- Trigeminal neuralgia
Helical Tomotherapy®
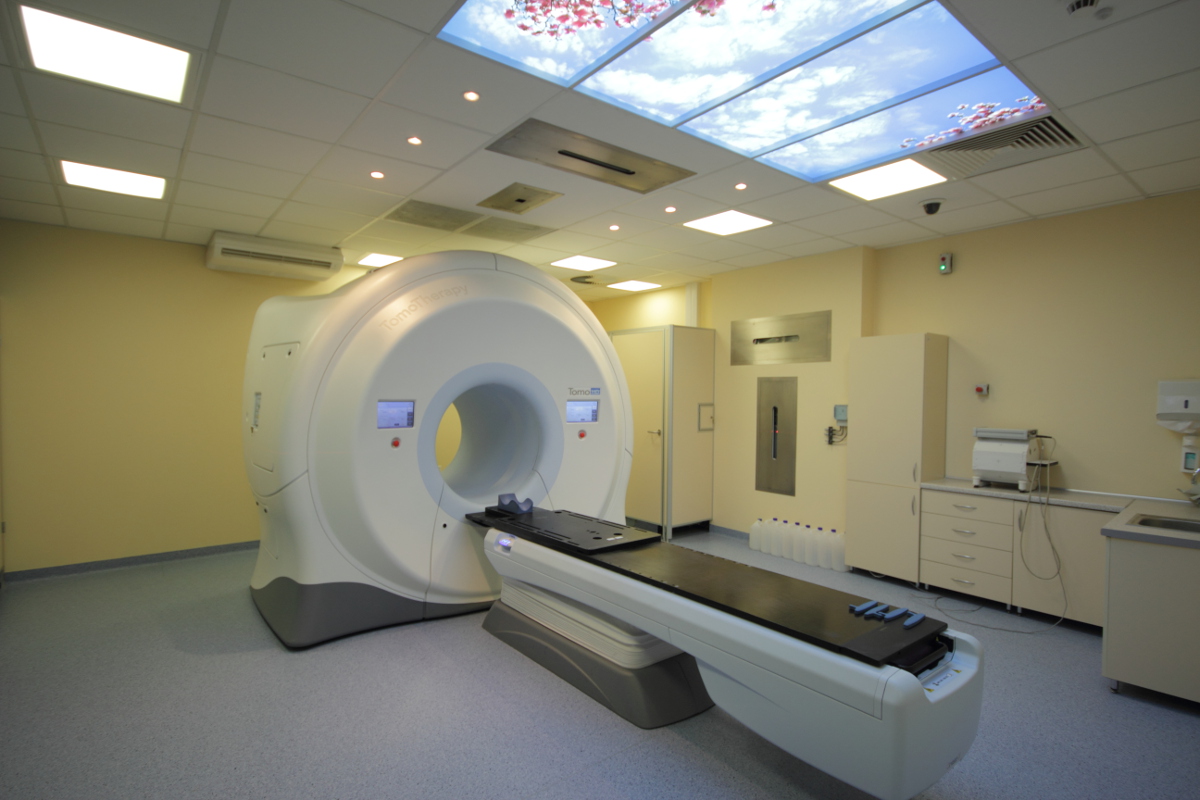 Tomotherapy represents yet another type of linac which can perform computed tomography. Its innovation consists in the ability to perform a megavoltage CT directly in the treatment room. The CT scans are used to check the patient's actual position vs the planned one and, in case of variances, the patient’s position may be adjusted using a routing table. In some cases it is possible to develop a treatment plan based on computed tomography (MVCT).
Tomotherapy represents yet another type of linac which can perform computed tomography. Its innovation consists in the ability to perform a megavoltage CT directly in the treatment room. The CT scans are used to check the patient's actual position vs the planned one and, in case of variances, the patient’s position may be adjusted using a routing table. In some cases it is possible to develop a treatment plan based on computed tomography (MVCT).
Tomotherapy may be used for irradiation of tumors found in multiple locations. Each case is classified for this type of treatment following medical consultations.
Stereotactic radiosurgery and stereotactic body radiation therapy (SRS and SBRT)
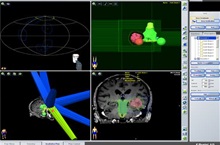
The word ‘radiosurgery’ consists of two parts: “radio” meaning the use of ionizing radiation and “surgery” (by analogy to the surgical treatment) meaning destruction of the tumor in a single procedure. The treatment does not entail physical removal of the tumor, however, as in the case of surgery; tumors are destroyed by irradiation instead. On the other hand, the stereotactic technique employs an external system of coordinates (usually a stereotactic frame), ensuring maximum precision for the tumor site. In modern radiosurgery systems, such as the CyberKnife, the tumor can be located without using a stereotactic frame, the reference system being the patient's anatomical structures (the so-called "internal coordinate system"). In some cases, the treatment may be divided into several sessions, or fractions, and the treatment is then called fractionated stereotactic radiotherapy. Fractionated stereotactic radiotherapy is the treatment of choice for tumors of considerable volume or located near organs easily damaged by ionizing radiation. By dividing the planned radiation dose into several fractions, the doctors can minimize the risk of any side effects while preserving high treatment efficiency. Stereotactic radiosurgery is used both for the treatment of brain tumors (intracranial radiosurgery) and tumors located in other parts of the body (extra-cranial radiosurgery). The most common indications for the application of the method include, among others, primary (meningioma, glioma) and secondary tumors of the brain (metastatic), pituitary adenoma, acoustic neuromas, early stage inoperative lung cancer, prostate cancer and single metastasis to the lung, liver, or the bone. Stereotactic radiosurgery is also used to treat certain non-cancerous diseases, such as cerebral vascular malformations or trigeminal neuralgia (trigeminalgia).
Gated radiation therapy
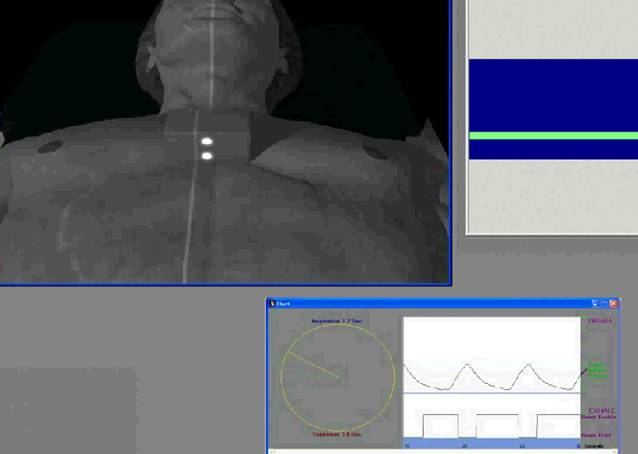 Respiratory gating is based on observing the patient's respiratory cycle during a radiotherapy session. The technique is used for irradiating tumors located in areas of significant respiratory motion, e.g. the lower part of the lung. The patient's respiratory movements are observed by locating external markers using an infrared camera system. The radiation oncologist determines the patient’s breathing pattern, pinpointing the moment when the therapeutic beam can be activated. In this method, irradiation takes place only when the tumor is located in a strictly defined position. Our Institute is at the forefront of this pioneering technology in Poland.
Respiratory gating is based on observing the patient's respiratory cycle during a radiotherapy session. The technique is used for irradiating tumors located in areas of significant respiratory motion, e.g. the lower part of the lung. The patient's respiratory movements are observed by locating external markers using an infrared camera system. The radiation oncologist determines the patient’s breathing pattern, pinpointing the moment when the therapeutic beam can be activated. In this method, irradiation takes place only when the tumor is located in a strictly defined position. Our Institute is at the forefront of this pioneering technology in Poland.
Volumetric Modulated Arc Therapy (VMAT)
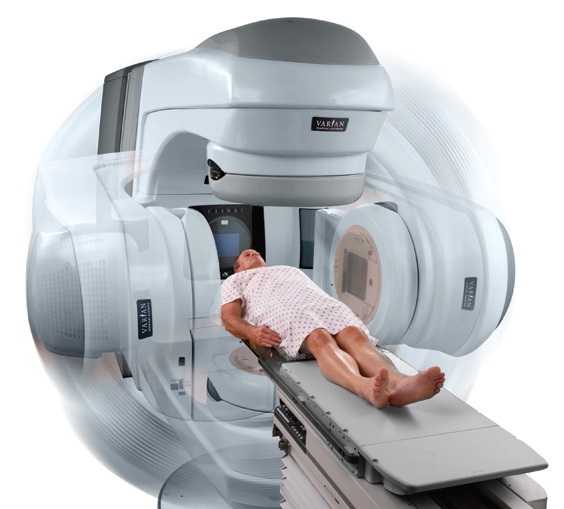
RapidArc, or volumetric modulated arc therapy (VMAT), is a dynamic technique performed by using a multileaf collimator, a variable dose rate, and a gantry rotation around the patient. It combines the arc and IMRT techniques and is characterized by a relatively shorter single radiotherapy treatment session compared with other available methods. Our Institute has pioneered this technology in Poland.
Total Skin Irradiation (TSI)
Irradiation of the whole skin (Total Skin Irradiation or TSI) represents a specific type of radiotherapy realized by an electron beam generated in the linac; hence its other name, Total Skin Electron Irradiation or TSEI. The treatment is used for certain specific forms of cutaneous T-cell lymphoma, such as mycosis fungoides or Sezary syndrome. The patient is irradiated while standing at a certain distance from the apparatus so as to irradiate maximum area of the skin. Irradiating other skin areas requires the patient to change his position. The treatment is continuously monitored by the physician and medical physicists who adjust the radiation beam parameters according to the position and the size of the patient's body.
Total Lymphoid Irradiation (TLI)
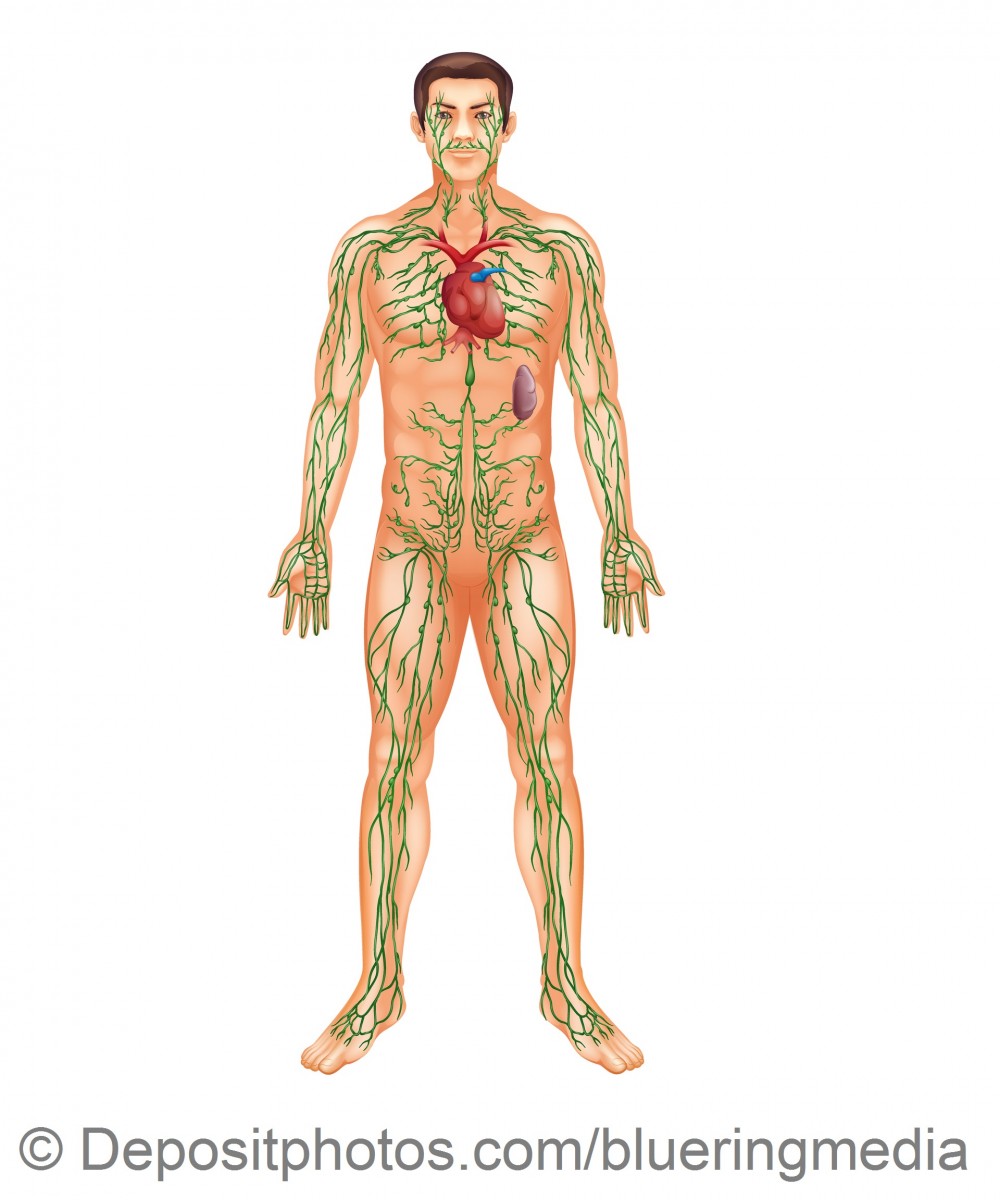 A highly specialized method of radiotherapy, TLI involves irradiation of the lymphatic chains: lymph nodes (cervical, axillary, mediastinal, retroperitoneal, pelvic, and inguinal), the spleen and tonsils (palatine, trumpet, throat, and tongue, which constitute the so-called Waldeyer's ring). This type of radiation therapy is used in some of the patients undergoing transplantation procedures: in some situations (usually to prevent transplant rejection) after organ transplantation of the heart, lung, or kidney, and in selected patients with certain cancers of the lymphatic system (as part of preparing the cells for bone marrow transplantation).
A highly specialized method of radiotherapy, TLI involves irradiation of the lymphatic chains: lymph nodes (cervical, axillary, mediastinal, retroperitoneal, pelvic, and inguinal), the spleen and tonsils (palatine, trumpet, throat, and tongue, which constitute the so-called Waldeyer's ring). This type of radiation therapy is used in some of the patients undergoing transplantation procedures: in some situations (usually to prevent transplant rejection) after organ transplantation of the heart, lung, or kidney, and in selected patients with certain cancers of the lymphatic system (as part of preparing the cells for bone marrow transplantation).
The treatment is carried out using modern accelerators that allow for rotary technique irradiation of large areas of the body (Tomotherapy equipment and the latest versions of the accelerator equipped with a RapidArc system). Each of them modulates the radiation beam while the radiation source rotates around the patient, allowing for delivery of a planned dose to the lymphatic system while sparing the organs that do not need radiotherapy. The TLI procedure is combined with TSI in selected patients presenting mycosis fungoides or Sezary syndrome, who are being treated in a clinical trial conducted by the Department of Bone Marrow Transplantation and Oncohematology and the Department of Radiotherapy.
Total Marrow Irradiation (TMI)
 One of the most advanced procedures for patients undergoing stem cell transplantation, TMI aims at destroying bone marrow cells in patients with hematologic malignancies (leukemias and lymphomas). The procedure is performed using Tomotherapy, or an accelerator permitting enforcement CT immediately prior to administering a therapeutic dose. The patient is positioned in a special vacuum bag on the therapeutic table. Before activating the radiation beam, the position of the patient is verified using CT for precise treatment plan parameters. TMI allows for delivery of precisely focused radiation to major marrow sites presenting cancer cells while sparing any surrounding tissues and organs, in particular the brain, lenses, mouth, lungs, heart, liver, kidney, intestines, and urinary bladder. In Poland, only the Cancer Centre in Gliwice currently performs this procedure!
One of the most advanced procedures for patients undergoing stem cell transplantation, TMI aims at destroying bone marrow cells in patients with hematologic malignancies (leukemias and lymphomas). The procedure is performed using Tomotherapy, or an accelerator permitting enforcement CT immediately prior to administering a therapeutic dose. The patient is positioned in a special vacuum bag on the therapeutic table. Before activating the radiation beam, the position of the patient is verified using CT for precise treatment plan parameters. TMI allows for delivery of precisely focused radiation to major marrow sites presenting cancer cells while sparing any surrounding tissues and organs, in particular the brain, lenses, mouth, lungs, heart, liver, kidney, intestines, and urinary bladder. In Poland, only the Cancer Centre in Gliwice currently performs this procedure!
Totab Body Irradiation (TBI)
One of the procedures for patients undergoing stem cells transplantation, TBI consists in destruction of the bone marrow cells in patients presenting hematologic malignancies (leukemias and lymphomas). During irradiation the patient first lies on one and then on his other side at a certain distance from the radiation source, with detectors placed on his body for medical physicists to properly adjust the radiation dose. The patient is also covered with special guards to protect his critical organs. Prior to the start of the procedure, the patient is photographed to ensure that his critical organs are sufficiently shielded. The treatment takes several sessions (usually three).
Image Guided Radiation Therapy (IGRT)
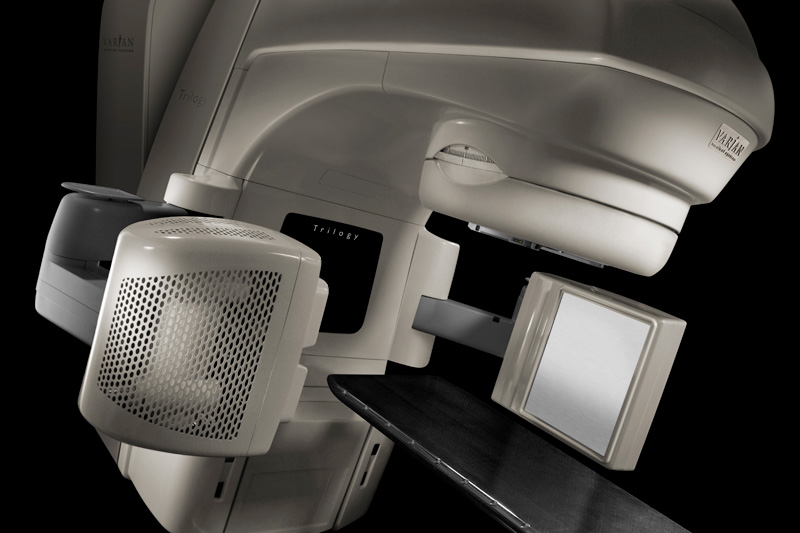
IGRT is a highly specialized procedure using 2D and 3D imaging (X-ray or ultrasound) during a radiation treatment cycle to direct radiation therapy to the tumor utilizing the imaging coordinates of the actual radiation treatment plan. Checking and adjusting the patient’s position (or a target volume) consists in comparing the actual images which were taken in the treatment room with reference images defined in the treatment planning system. Prior to starting the irradiation, a radiographer or a doctor checks and - if necessary - adjusts the patient’s position. Our Institute has pioneered this technology in Poland.
Intensity Modulated Radiation Therapy (IMRT)

The radiotherapy technique utilized by the multileaf collimator (MLC) allows for any dose painting of the tumor and the surrounding tissues. IMRT radiotherapy is also called slotted radiotherapy because the dose is delivered by continuous opening and closing of the leaves in the treated area. Our Institute has pioneered this technology in Poland.
Intraoperative Radiation Therapy (IORT)
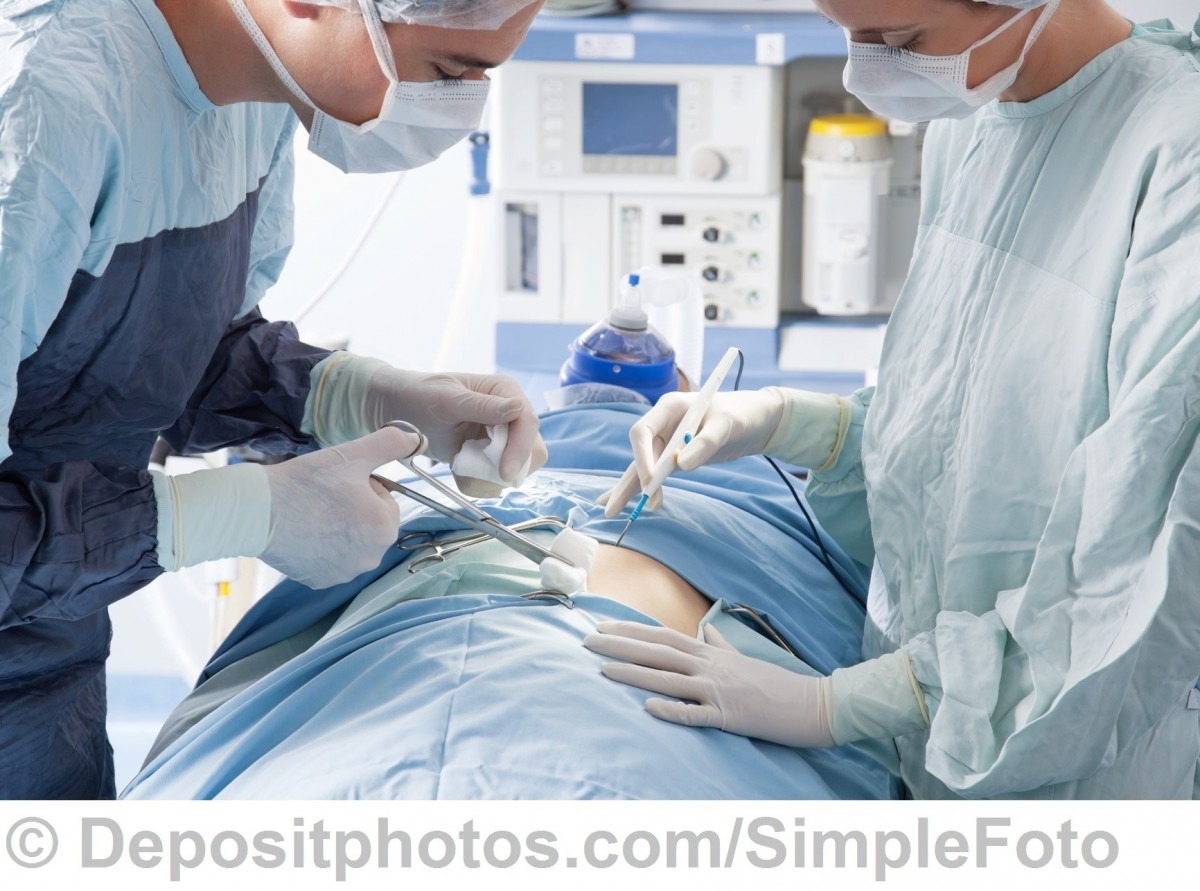
Intraoperative Radiotherapy is performed during surgery. Irradiation is applied after removing the tumor together with a resection margin, i.e. a portion of the surrounding healthy tissue. This procedure uses a special intraoperative radiotherapy machine and consists in precise and focused irradiation of the site from which the tumor has been excised, and destroying any potentially remaining cancer cells. Our Institute has pioneered this technology in Poland.
Hyperthermia and Hyperthermia Combined with Radiotherapy
 Hyperthermia is a treatment of malignancies which uses an external heat source to raise the tumor temperature above 40°C. The high temperature affects the tumor in several ways, of which the most significant are an individual cytotoxic effect, improvement of microcirculation and tumor perfusion, protein aggregation in a tumor cell, and tumor DNA replication delay. Hyperthermia is used as a stand-alone method, a radiosensitizer or in combination with radiotherapy. For superficial hyperthermia treatment, the Department of Radiotherapy in Gliwice uses a BSD 500 device which utilizes microwave generators to raise tissue temperature. Hyperthermia treatment must incorporate proper temperature control using thermometers placed on the skin and subcutaneously; hence, it is often necessary to perform subcutaneous application of the guide under local anesthesia. Hyperthermia treatment takes about 60 minutes and is usually combined with palliative radiotherapy, with the exact program defined by the attending physician. It usually consists of two or three sessions prior to radiotherapy fractions. Hyperthermia is much less frequently used: mostly when it is not possible to re-irradiate the treated area. Superficial hyperthermia is the treatment of choice for patients presenting tumors in the skin, e.g. metastases, primary tumors, recurrent cancers, sarcomas, and melanomas; in the subcutaneous tissue, and other superficial tumors of other soft tissues without extensive tumor ulcerations (because high temperature intensifies necrosis and ulceration). The final decision as to whether the patient qualifies for the treatment, as well as the treatment regimen, is the purview of the attending physician of the Department of Radiotherapy.
Hyperthermia is a treatment of malignancies which uses an external heat source to raise the tumor temperature above 40°C. The high temperature affects the tumor in several ways, of which the most significant are an individual cytotoxic effect, improvement of microcirculation and tumor perfusion, protein aggregation in a tumor cell, and tumor DNA replication delay. Hyperthermia is used as a stand-alone method, a radiosensitizer or in combination with radiotherapy. For superficial hyperthermia treatment, the Department of Radiotherapy in Gliwice uses a BSD 500 device which utilizes microwave generators to raise tissue temperature. Hyperthermia treatment must incorporate proper temperature control using thermometers placed on the skin and subcutaneously; hence, it is often necessary to perform subcutaneous application of the guide under local anesthesia. Hyperthermia treatment takes about 60 minutes and is usually combined with palliative radiotherapy, with the exact program defined by the attending physician. It usually consists of two or three sessions prior to radiotherapy fractions. Hyperthermia is much less frequently used: mostly when it is not possible to re-irradiate the treated area. Superficial hyperthermia is the treatment of choice for patients presenting tumors in the skin, e.g. metastases, primary tumors, recurrent cancers, sarcomas, and melanomas; in the subcutaneous tissue, and other superficial tumors of other soft tissues without extensive tumor ulcerations (because high temperature intensifies necrosis and ulceration). The final decision as to whether the patient qualifies for the treatment, as well as the treatment regimen, is the purview of the attending physician of the Department of Radiotherapy.
Three-Dimensional Conformal Radiation Therapy (3DCRT)
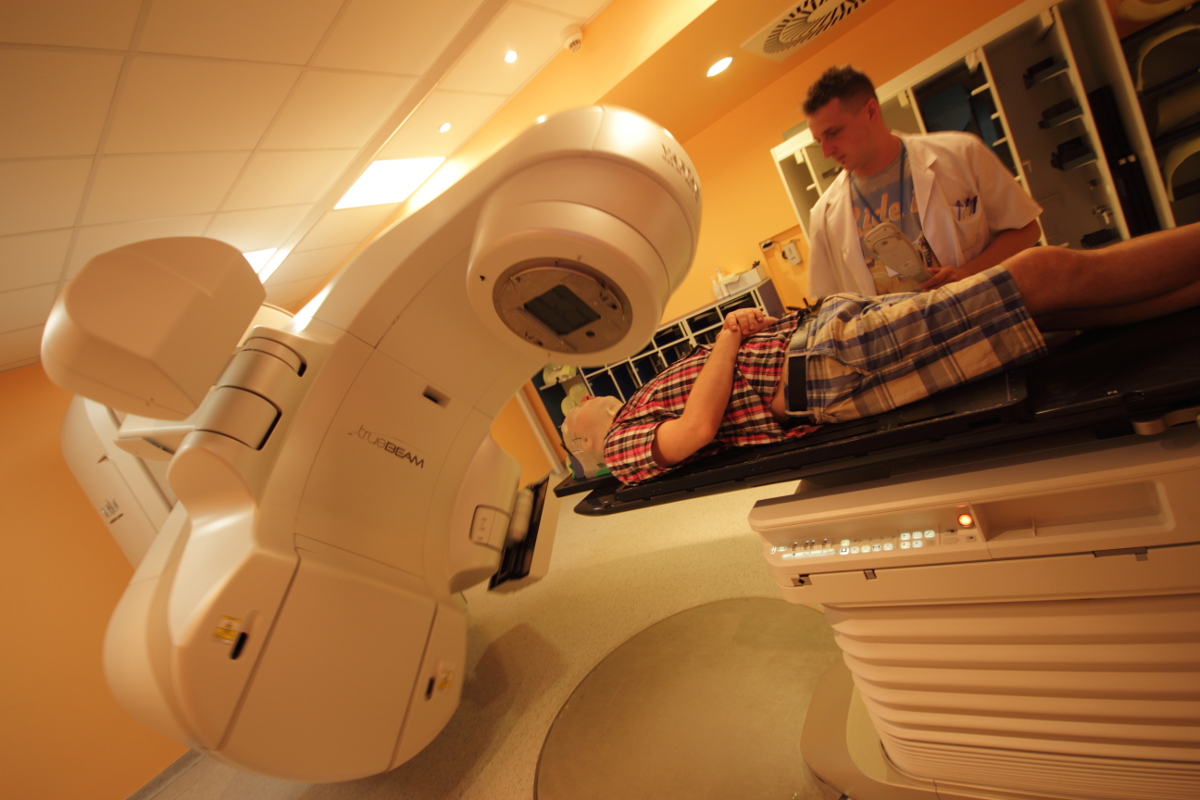
During tele-radiotherapy an external beam of high-energy X-rays is generated by a linear accelerator to irradiate and destroy the tumor. The treatment continues for 5 days a week (from Monday to Friday) for several weeks, thus providing an overall dose to the tumor area sufficiently high to destroy all the cancer cells, while the intervals between successive radiotherapy fractions allow enough time for the surrounding healthy tissue to regenerate. Since tumors are irregular in shape and size, treatment planning is done using special imaging techniques, such as computed tomography (CT), magnetic resonance imaging (MRI), or PET. For most patients, treatment planning begins with preparing a thermoplastic mask (orfit mask). The resulting immobilization allows for CT or PET testing to be performed to show the tumor in three planes: transverse, sagittal, and coronal. When injection of contrast is required during the CT scan, the patient is instructed not to eat for approximately 6 hours prior to the test and to bring his serum creatinine test result. Images obtained during the tests are uploaded to a special planning system where a medical physicist defines the radiation beam and the irradiation field in order to match the size and shape to the irradiated tumor while protecting the surrounding healthy tissue, or so-called critical organs. After the treatment plan has been developed and approved by the radiation oncologist, a so-called simulation is performed, in which relevant reference points are marked on the thermoplastic hood. In order to improve the precision of the treatment, the correct positioning of the patient is verified prior to each individual fraction delivery by means of image guided radiation therapy systems. Administration of a single fraction takes several minutes while the patient is lying in a comfortable position. Throughout the entire treatment cycle, however, the patient may experience both immediate and delayed side effects, which the attending physician will discuss with him prior to the initiation of radiotherapy.
Radiotherapy of Non-malignant Diseases
 Many non-malignant diseases, particularly those accompanied by painful inflammatory processes, respond well to ionizing radiation. The radiotherapy applied in such cases is more complex than in the case of tumors. It is characterized by the lack of a clear effect of the fractionated dose volume, which allows for the application of small, safe fractional and total doses without the risk of a post-radiation reaction. Among diseases susceptible to radiation therapy, the largest group consists of painful orthopedic conditions or conditions accompanied by pathological fibrosis and ossification, such as:
Many non-malignant diseases, particularly those accompanied by painful inflammatory processes, respond well to ionizing radiation. The radiotherapy applied in such cases is more complex than in the case of tumors. It is characterized by the lack of a clear effect of the fractionated dose volume, which allows for the application of small, safe fractional and total doses without the risk of a post-radiation reaction. Among diseases susceptible to radiation therapy, the largest group consists of painful orthopedic conditions or conditions accompanied by pathological fibrosis and ossification, such as:
- - Painful shoulder syndrome
- - Elbow pain syndrome (also called tennis elbow)
- - Inflammation of the plantar fascia of the foot (the so-called heel spurs)
- - Dupuytren's disease (palmar fascia contracture)
- - Prevention of pathological heterotopic ossification (e.g. following hip arthroplasty)
- - Inflammation of the Achilles tendon.
Half Body Irradiation (HBI

HBI represents another method of irradiation treatment of patients presenting multiple cancer metastases to the bones which have been confirmed by performing scintigraphy, CT, or MR imaging. In order to expand the size of the irradiation field, the patient is placed on a Styrofoam board rather than on a therapeutic table placed on the floor of the treatment room. The dose generated by the accelerator is measured by semiconductor detectors placed at several locations on the patient's skin. Treatment involves two opposing fields: anterior-posterior and posterior-anterior. The dose to the upper half of the body is reduced to 6 Gy, while the radiation dose for the lower body is reduced to 8 Gy. HBI avoids combining multiple fields, shortens the treatment time, and assures a more homogeneous dose distribution than conventional treatment. The reduced treatment time is particularly important for patients in general serious condition and patients experiencing severe pain. This type of treatment helps reduce pain and usually leads to overall general improvement.







 Polski
Polski





